CORNEAL CARE

CORNEAL GRAFTING: A Brief Introduction
Corneal diseases are the second C most prevalent cause of blindness and according to WHO affect more than 10 million people worldwide. In India some 20,000 people have corneal transplants each year.
Corneal transplantation for corneal pathologies has a long history, and has enjoyed a relatively high success rate as compared with transplantation of other tissues. Corneal transplantation has evolved rapidly over the past decade, as surgeons attempt to refine selective tissue transplantation to treat diseases that affect specific layers of the cornea.
Although full thickness penetrating keratoplasty has been more popular than lamellar keratoplasty traditionally, the techniques for lamellar keratoplasty have advanced dramatically. At present, posterior lamellar (endothelial) keratoplasty is the treatment of choice for corneal endothelial disease, and deep anterior lamellar keratoplasty is strongly advocated for corneal stromal disease.
In this issue will help you and your family understand corneal transplant surgery and explain what you need to know during the recovery period.
This issue also presents few interesting clinical cases related to corneal transplantation. Please take time to read this information and save it for future.
Corneal transplantation for corneal pathologies has a long history, and has enjoyed a relatively high success rate as compared with transplantation of other tissues. Corneal transplantation has evolved rapidly over the past decade, as surgeons attempt to refine selective tissue transplantation to treat diseases that affect specific layers of the cornea.
Although full thickness penetrating keratoplasty has been more popular than lamellar keratoplasty traditionally, the techniques for lamellar keratoplasty have advanced dramatically. At present, posterior lamellar (endothelial) keratoplasty is the treatment of choice for corneal endothelial disease, and deep anterior lamellar keratoplasty is strongly advocated for corneal stromal disease.
In this issue will help you and your family understand corneal transplant surgery and explain what you need to know during the recovery period.
This issue also presents few interesting clinical cases related to corneal transplantation. Please take time to read this information and save it for future.
What Is Cornea
The cornea is the transparent, domeshaped window covering the front of the eye like the crystal on a watch, it gives us a clear window to look through. Because there are no blood vessels in the cornea, it is normally clear and has a shiny surface. It is a powerful refracting surface, providing 2/3 of the eye's focusing power.
In humans, the cornea has a diameter of about 11.5 mm and a thickness of 500600 m in the center and 600–800 m at the periphery. Transparency, avascularity, the presence of immature resident immune cells, and immunologic privilege makes the cornea a very special tissue. It is comprised of 5 layers.
In humans, the cornea has a diameter of about 11.5 mm and a thickness of 500600 m in the center and 600–800 m at the periphery. Transparency, avascularity, the presence of immature resident immune cells, and immunologic privilege makes the cornea a very special tissue. It is comprised of 5 layers.
LASER ASSISTED TRANSPLANT
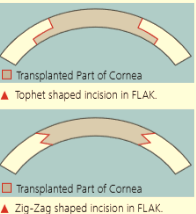
FLAK-Femtosecond Laser Assisted Keratoplasty
Femtosecond Laser Assisted Keratoplasty (FLAK) yields visual comparable to PKP but with better healing and graft strength.
FLAK provides better outcomes in terms of astigmatism, visual acuity and early visual recovery than conventional penetrating keratoplasty. What makes the femtosecond laser appealing in keratoplasty is its ability to incise corneal tissue with greater precision and accuracy than hand trephination and to achieve interlocking edges in the graft-host interface that are not possible by hand. More advanced uses of the femtosecond laser are moving beyond fullthickness keratoplasty and into posterior lamellar incisions for Descemet's stripping automated endothelial keratoplasty (DSAEK), Descemet's membrane endothelial keratoplasty (DMEK), anterior lamellar keratoplasty (ALK) without sutures, deep anterior lamellar keratoplasty (DALK) and astigmatic keratotomies.
Tophat shaped incision can help restore a more regular corneal surface if there is thinning in the area where the incision will be made.
Interlocking incisions for DALK to create a strong seal between the donor and recipient tissue. The zigzag shaped incision is particularly useful for DALK.
FLAK provides better outcomes in terms of astigmatism, visual acuity and early visual recovery than conventional penetrating keratoplasty. What makes the femtosecond laser appealing in keratoplasty is its ability to incise corneal tissue with greater precision and accuracy than hand trephination and to achieve interlocking edges in the graft-host interface that are not possible by hand. More advanced uses of the femtosecond laser are moving beyond fullthickness keratoplasty and into posterior lamellar incisions for Descemet's stripping automated endothelial keratoplasty (DSAEK), Descemet's membrane endothelial keratoplasty (DMEK), anterior lamellar keratoplasty (ALK) without sutures, deep anterior lamellar keratoplasty (DALK) and astigmatic keratotomies.
Tophat shaped incision can help restore a more regular corneal surface if there is thinning in the area where the incision will be made.
Interlocking incisions for DALK to create a strong seal between the donor and recipient tissue. The zigzag shaped incision is particularly useful for DALK.
Things To Expect
- You will be in the operating room for 1-2 hours, but the actual surgery takes less time
- Following surgery, your eye most likely will be red, irritated, and sensitive to light
- Discomfort usually is controlled with topical drops.
- Most people will have sutures, although you probably will not be aware of them.
- Some sutures may be removed as early as three months after surgery. Others may remain for a year or more.
- Vision usually is blurred after surgery. It gradually improves as healing takes place. You may need to wait for 3 to 12 months for new glass prescription.
- Some patients with desk jobs can return to work within a few days. Other can be off work for a few weeks.
- The risk of corneal transplant rejection is low. However, it is possible to have a rejection at any time even many years after your transplant surgery.
Corneal Transplant
If the cornea becomes distorted in shape, scarred, or hazy (opaque) from disease or injury, the light rays passing through it are distorted and the vision is reduced.
A corneal graft (transplant) may be necessary to replace the diseased or injured cornea with a healthy, clear cornea to restore good vision. This operation is also known as a keratoplasty, and involves the replacement of part or all of your cornea with human donor tissue.
A corneal graft (transplant) may be necessary to replace the diseased or injured cornea with a healthy, clear cornea to restore good vision. This operation is also known as a keratoplasty, and involves the replacement of part or all of your cornea with human donor tissue.
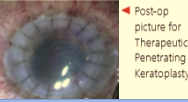
Penetrating Keratoplasty
During traditionalpenetrating keratoplasty (PK), a circular button-shaped, full-thickness section of tissue is removed from the diseased cornea using either a surgical instrument called a trephine or a femtosecond laser.
A matching "button" from the donor tissue is then positioned and sutured into place. The sutures (stitches) remain in place typically for a year or more after surgery. Corneal transplants are performed on an outpatient basis and it generally takes one to two hours, meaning you can go home a short while after the surgery (though you will need someone to drive you home). Because of the cornea’s lack of blood supply, healing takes place very slowly.
Restoration of vision after corneal transplant surgery is gradual. The vision in the operated eye will be somewhat blurred and distorted until final glasses or contact lenses are prescribed. This is a sight-saving surgery, but it also requires patients and ophthalmologists to work closely together to insure the success of the surgery.
A matching "button" from the donor tissue is then positioned and sutured into place. The sutures (stitches) remain in place typically for a year or more after surgery. Corneal transplants are performed on an outpatient basis and it generally takes one to two hours, meaning you can go home a short while after the surgery (though you will need someone to drive you home). Because of the cornea’s lack of blood supply, healing takes place very slowly.
Restoration of vision after corneal transplant surgery is gradual. The vision in the operated eye will be somewhat blurred and distorted until final glasses or contact lenses are prescribed. This is a sight-saving surgery, but it also requires patients and ophthalmologists to work closely together to insure the success of the surgery.
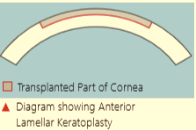
Lamellar Keratoplasty
In ALK, we dissects the cornea into two thin pieces and removes the front, scarred part. A matching area of tissue from a donor cornea is then used to replace the area that was removed. Donar cornea is than sutured into place with continuous or interpret sutures.
It’s a type of ALK known in which the surgeon only leaves behind 5% or less of your original corneal thickness and replaces the rest with donor tissue. DALK surgery can be done with a manual or hand dissection of donor tissue. Best it is done by using air to detach the inner layer of your cornea with a technique called the “big bubble” technique.
DALK is our treatment of choice for keratoconus or corneal scars, as long as the inner cell layer of the cornea (the endothelium) is healthy.
It’s a type of ALK known in which the surgeon only leaves behind 5% or less of your original corneal thickness and replaces the rest with donor tissue. DALK surgery can be done with a manual or hand dissection of donor tissue. Best it is done by using air to detach the inner layer of your cornea with a technique called the “big bubble” technique.
DALK is our treatment of choice for keratoconus or corneal scars, as long as the inner cell layer of the cornea (the endothelium) is healthy.
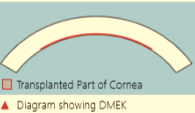
Endothelial Keratoplasty
Endothelial Keratoplasty is the preferred way to restore vision when the inner cell layer of the cornea stops working properly from Fuchs’ dystrophy, bullous keratopathy, iridocorneal endothelial (ICE) syndrome, or other endothelial disorders. In the EK procedure, the surgeon removes the diseased inner cell layer of the cornea and implants healthy donor tissue through a small incision An air bubble is used to unfold and position the donor tissue against the patient’s cornea The small incision is either self-sealing or may be closed with a few sutures
Advantages of Endothelial Keratoplasty over Peneterating Keratoplasty
Advantages of Endothelial Keratoplasty over Peneterating Keratoplasty
Less operating time and faster recovery. Minimal removal of corneal tissue (and therefore less impact on the structural integrity of the eye). No suture related complications. Reduced risk of astigmatism after surgery.

International Quality Accreditated by
Joint Commission International, USA (JCI)
Online Appointment
Book Online Appointment and Save 10% on Online Payment.
